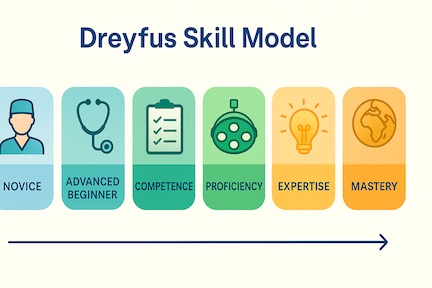
The Dreyfus model of skill acquisition was proposed in 1980 and has since been used by educators to explain how learners progress from being novices to becoming experts, passing through stages of being an advanced beginner, competent, and proficient at their assigned task. The authors later added a sixth stage, that of master, to their sequential and somewhat linear progression scale.
The model is intuitively logical and appears to apply to most professional learning endeavors. It suggests that as learners progress, they move from strictly applying rules and guidelines to becoming aware of how their actions might affect and be affected by circumstances and their environment. This “intuitive perspective,” once acquired, is an important aspect of competence. With further work, training, and experience, learners develop what is referred to as “reflexive reorientation,” whereby learners are able to competently respond to changing or unexpected situations without necessarily resorting to reflective decision-making. For the most part, this defines the “expert” level of skill development.
The question is whether the Dreyfus model lends itself clearly to learning interventional pulmonology. Considering how the model stresses the importance of rules, guidelines, and intuitive experience-based decision-making, it helps educators design competency-oriented curricula and develop step-by-step knowledge and skills-related learning and testing materials. It underscores the importance of experiential knowledge and thus reinforces the complementarity of apprentice-style training with simulation-based learning.
The drawbacks, especially as regards bronchoscopy and interventional pulmonology, are based on the fact that one can reside simultaneously in different stages for different procedures, all while being perceived as an expert overall based on certification, place of practice, presumed experience, or academic titles. Furthermore, the boundaries between stages are blurred, and one may progress, regress, plateau, or skip stages depending on clinical context, the degree of technical difficulty of the procedure, or the complexity of the patient’s circumstances and medical environment. By no means, therefore, is there a linear progression universally applicable to all aspects of IP.
Considering these limitations, I wonder whether a limited certification process could be helpful for certain groups of procedures. Obviously, competency-oriented learning materials for each group would address technical, cognitive, affective, and experiential knowledge, complemented by a series of associated assessment tools, simulation-based exercises, and real-life training experiences that help determine competency and level of expertise.
The model also fails to consider individual learning differences, cultural variances, or the importance of having access to experts and masters for guidance and assistance. It ignores differences in experiential training, personality, and decision-making skills that might empower or endanger the effects of intuitive thinking and reflective reorientation, or reinforce personal biases that might hinder rather than promote professional and personal growth. I believe these elements become especially important for those aspiring to practice at the expert level.
